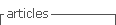INTRODUCTION
Antibiotics have saved millions of lives, and have also brought a revolution in medicine. However, a growing threat impairs the efficacy of these drugs: bacterial resistance to antibiotics, which is defined as the ability of a bacterium to survive antibiotic concentrations that inhibit/kill others of the same species1. Bacterial resistance to antibiotics is a serious public health problem that is becoming increasingly complex to deal with2. The increase in microbial resistance due to the selective pressure represented by the use of antibiotics on a large scale, especially in our hospitals, has allowed the selection of strains with resistance mechanisms that, on many occasions, leave us practically without alternatives for the treatment of infections3,4. South America is one of the regions most affected by resistance to penicillin, according to data from the epidemiological surveillance of the SIREVA group coordinated by the Pan American Health Organization 5.
This study aims to describe the resistance profile of S. aureus colonizing the oral cavity of patients who attended the Clinical Dental Surgery Department, at the Faculty of Dentistry of the National University of Caaguazú, in the city of Coronel, Oviedo, Paraguay, between the months of august and September 2021. During this period data was collected and samples were taken to send them to the laboratory of the Regional Health Research Institute (IRIS) where they were processed.
The most representative species in the oral cavity is S. aureus, its presence as a component of the oral microbiota is controversial and may be associated with endodontic, periodontal, periapical infections, and suppurative infections of the salivary glands, under dentures, and in immunocompromised patients4. Currently, all S. aureus isolates of hospital origin and more than 85% of those of community origin are resistant to penicillin5. The presence is a risk factor for the development of bacterial endocarditis and other infections6,7. International organizations have highlighted the importance of monitoring antibiotic resistance and its causes as an essential measure to prevent its spread8,9. We aimed to determine the resistance to antibiotics in S. aureus from the oral cavity of patients who attended a public clinic for treatment.
In the literature there are few studies about the distribution of Staphylococcus spp in the mouth and those that exist as residents of the oral cavity are controversial. The genus Staphylococcus spp forms an important group of pathogens in humans and causes different diseases, including Infectious endocarditis. Furthermore, the literature reports rates of resistance to amoxicillin and clindamycin antibiotics commonly used for prophylaxis in dentistry10.
METHODS
Design and population: Observational, descriptive cross-sectional study with non-probabilistic sampling of consecutive cases. Patients who attended the FOUNCA Dental Clinic on Wednesday mornings in 2021 were included according to the inclusion criteria. The context of the study in time and space was the most appropriate for the type of study carried out. Those who did not provide their informed consent, who had received antibiotics in the last 15 days, and those who did not provide the necessary clinical data to complete the epidemiological clinical record designed for this work were excluded.
A standardized questionnaire was used to collect patients’ information; in which sociodemographic data and questions related to risk factors associated with S. aureus were included. Some information, such as: i) the use of antibiotics in the last 3 months, ii) severe skin infection that has required treatment at home or by a medical professional in the last 3 months, iii) skin infections in last 6 months, iv) abscesses and ulcers with pus were also surveyed. Family history of infections and other personal history such as underlying pathologies like immunodeficiency, heart disease, nephropathy, chronic skin pathology, lung disease and previous hospitalization. The presence of S. aureus was measured as the main variable and its resistance to different antibiotics: cefoxitin, oxacillin, vancomycin, erythromycin, ciprofloxacin.
Outcomes: The presence of S. aureus and its sensitivity to 11 antibiotics were measured as the main variable.
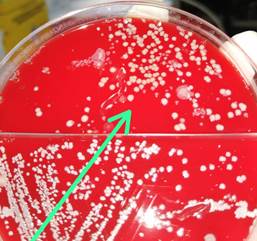
Microbiological analysis: Sampling from the oral cavity was carried out with sterile swabs. The samples were transported in a thioglycolate medium and cultured on salty mannitol agar. Mannitol-positive colonies were cultured on blood agar, identifying S. aureus by conventional biochemical tests that included positive results for catalase, coagulase, DNAse and latex agglutination test for S. aureus. The resistance study was performed using the disk diffusion method according to the Clinical and Laboratory Standards Institute (CLSI) and 11 antibiotics were included. The antibiotics used in the test were penicillin, cefoxitin, oxacillin, vancomycin, erythromycin, ciprofloxacin, clindamycin, rifampicin, trimethoprim, tetracycline, and gentamicin.
Statistical analysis. The data obtained from the study was stored using an Excel spreadsheet based on the questionnaire. The Stata 15.0 program was used to carry out descriptive analyses. Frequency and measures of central tendency were used.
Ethical and biosafety considerations: Informed consent was requested to participate in the study. The sampling procedure was non-invasive, so it did not entail discomfort or health risks for the participants. It was carried out using personal protective equipment and sterile materials. Patients were informed of the confidentiality of the information. The protocol 03/2021 was approved by the Ethics Board of the Universidad Nacional of Caaguazú.
RESULTS
A total of 43 patients participated in the study, 67.4% were female, the average age was 30 years old, 83.7% had oral pathologies, 6.9% had a history of hospitalization while 4.7% mentioned that they were exposed to S. aureus (Table 1).
Table 1. Demographic and clinical characteristics of the study participants. no:43.
| n (%) | |
|---|---|
| Sex | |
| Female | 29 (67.4) |
| Male | 14 (32.6) |
| Age | |
| 30 (21- 44) | |
| Personal history | |
| Yes | 10 (23.3) |
| No | 33 (76.7) |
| Family history | |
| Yes | 6 (13.9) |
| No | 37 (86.1) |
| Oral pathology | |
| Yes | 36 (83.7) |
| No | 7 (14.3) |
| Number of cavities | |
| 7 (5 -10) | |
| History of hospitalization | |
| Yes | 3 (6.9) |
| No | 40 (93.1) |
| Use of antibiotics | |
| Yes | 8 (18.6) |
| No | 35 (81.4) |
| Exposure to S. Aureus | |
| Yes | 2 (4.7) |
| No | 41 (95.4) |
We isolated S. aureus from three patients. One sample was resistant to a single antibiotic and two were resistant to two or more antibiotics.
Resistance to oxacillin, cefoxitin, erythromycin, clindamycin, and penicillin was found. S. aureus was isolated in 3 patients and 100% of the isolates, presented resistance to penicillin, while 2 of the three isolates were resistant to oxacillin and cefoxitin. Resistance to erythromycin and clindamycin was also present in only one of the strains. There was no resistance to tetracycline, rifampicin, gentamicin, trimethoprim Sulfamethoxazole and vancomycin (Table 2).
DISCUSSION
Russomando (2014), reported S. aureus in 37 samples of a total of 112 patients of which 35 (94.6%) presented resistance to at least one antibiotic. They were resistant to: Penicillin (89%), Chloramphenicol (16.2%), Oxacillin (10.8%), Erythromycin (8%), Clindamycin (8%), Gentamicin (5.4%) and one isolate with intermediate resistance to Ciprofloxacin (2.7%) (4). These results are like the resistance profile of S. aures isolated in our study. In this study S. aureus was reported in 3 samples of a total of 48 patients (6%) and all of them were resistant to at least one antibiotic. This showed that resistance to antibiotic of S. aureus is high.
Barrientos et al, in his study included 46 adult patients who attended the Stomatology and Cardiology service of HOCEN (Bogota, Colombia) during the month of August 2010 and that presented high risk of Infectious Endocarditis. Of the 46 patients, Staphylococcus spp. was identified in 28.2%. Of these, 61.5% was S. aureus, 30.7% S. epidermidis and 7.6% S. hominis. Of the Staphylococcus spp 30.8% were resistant to clindamycin and 76.9% to amoxicillin10.
The irrational use of antibiotics has become a common practice. In developing countries, antibiotics are prescribed to a large percentage of hospitalized patients and are often not needed. In addition, inappropriate self-medication of antibiotics exacerbates the situation. Since 2018, in Paraguay the law imposed that antibiotics could not be sold without a prescription. But the legacy of decades of irrational use of antibiotics leaves consequences in the community.
Knowing the resistance to antibiotics presented by bacteria in the oral cavity is the first step to implement oral health programs that prevent the appearance of resistant strains, control healthy carriers and formulate treatments that avoid future risks and reduce morbidity and mortality rates, especially by Endocarditis infection.
In a study by Marquez-Oviedo (2021) colonies of S. aureus of the oral mucosa showed resistance to penicillin. Of the 64 samples, the prevalence of sensitivity was 60% for amoxicillin/clavulanic acid, clotrimoxazole, gentamicin, oxacillin, ciprofloxacin, vancomycin, and ampicillin/sulbactam The prevalence of S. aureus from the oral mucosa was 7.8%, a result almost like our study11.
The detection of resistance to different types of antibiotics could jeopardize the future of antibiotic therapy as an adjunct to the treatment of periodontitis. An exhaustive monitoring of the evolution of resistance to antibiotics in the oral microbiota must be established, with the aim of building strategies to stop its increasing spread.
For this reason, surveillance of Antimicrobial Resistance (RAM) is necessary to have timely data that lead to relevant and rational treatments. These surveillance studies also allow to establish trends in a specific pathogen and, especially, to recognize emerging problems in the microorganisms under surveillance.
Bravo et al., in his study, stated that S. aureus are adaptable human pathogen, their pathogenic capacity with their virulence genes and their propensity to acquire resistance to antimicrobials, justify the evaluation of the presence of this microorganism in handpieces and mobile phone screens. This study reported that 40% of the strains presented the mecA gene, the tst gene was identified in 80% of the strains, while no strain had the lukS-F PV gene. In conclusion, resistant and virulent strains of S. aureus were found on mobile phone screens and high-speed parts of dental offices12.
Some limitations in our study were the number of patients who attended the clinic, the patients who had consumed antibiotics in the last fifteen days, some people unwilling to participate in the study. The scope of this study implies greater health surveillance from the Ministry of Public Health and Social Welfare, given this, its importance lies in preventing more serious causes of resistance that would prevent the correct actions of antibiotics in humans. The high level of resistance to penicillin, oxacillin and cefoxitin must be taken into account, as reported in other researches, which implies a high risk that deserves health surveillance.
CONCLUSIONS
In this study a greater number (67%) of female patients was detected, a high percentage of the study population had oral pathologies, 6.9% of those who attended the clinics of the Faculty of Dentistry of the National University of Caaguazú (FOUNCA), had the carriage of S. aureus in the oral cavity, these were resistant to one or more antibiotics. Some patients without risk factors such as previous hospitalization or consumption of antibiotics resulted with S. aureus resistant to penicillin.